When Recurrent UTIs Turn Into Vulvodynia: A Doctor’s Personal Story
By a physician and patient
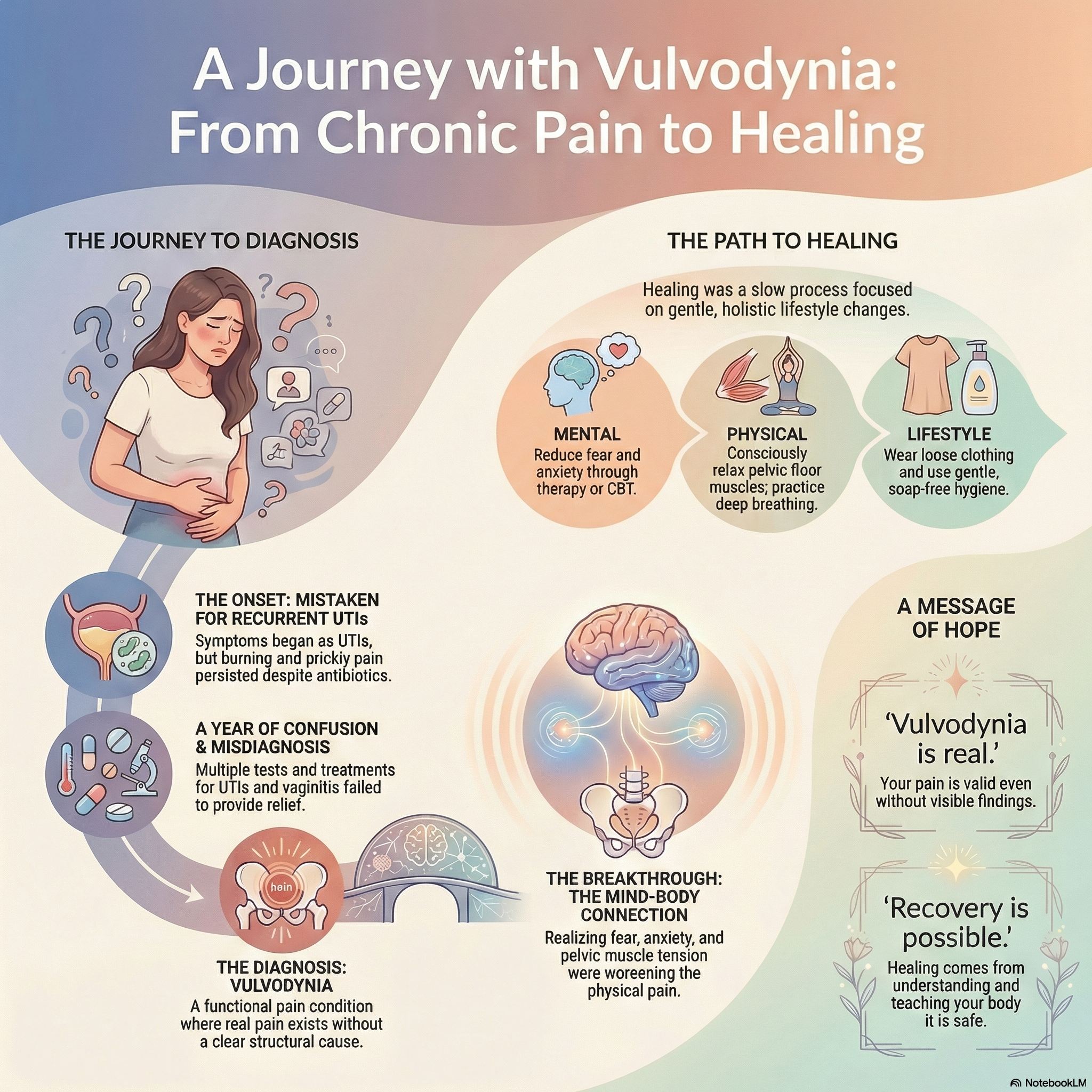
I developed recurrent urinary tract infections after intercourse for a few months. Each time, I took antibiotics and felt better. But in 2023, one episode became different. The symptoms didn’t resolve, even after antibiotics.
I started feeling burning, prickly, itchy sensations on my vulva, especially after passing urine. I couldn’t tell whether it was a UTI or vaginitis. Being a doctor, my first thought was antibiotic resistance, so I escalated treatment. Still, the symptoms continued.
Urine routine tests showed no infection, but cultures grew bacteria with sensitivity reports. I took antibiotics accordingly—yet nothing changed. I consulted a gynecologist, thinking it might be vaginitis. That began a year-long cycle of repeated gynecology visits, urine cultures, vaginal swabs, and multiple antibiotics for presumed UTIs and vaginitis.
After more than a year, I finally met a gynecologist who diagnosed me with vulvodynia.
Unfortunately, vulvodynia is barely taught in medical training. Even with a diagnosis, there was no clear treatment plan. I searched online and tried everything I could find. I stopped antibiotics, creams, gels, and lotions. I avoided tight clothing and undergarments. My symptoms reduced—but never completely disappeared.
Then I stopped talking about it.
People didn’t understand, and I didn’t feel understood. Intercourse became painful, so I avoided it. Anxiety about conceiving grew. Carrying pain silently, combined with fear and frustration, took a toll on my mental health. I was constantly anxious and crying, yet afraid to read more—scared I’d discover there was no cure and that this would last forever.
After 1.5 years, I finally gathered the courage to learn more. Patient blogs and forums helped me feel less alone. I remembered my gynecologist mentioning cognitive behavioral therapy (CBT) and began reading about how fear, anxiety, and pelvic muscle tension can worsen vulvodynia.
That changed everything.
Vulvodynia is a functional condition, much like IBS. There may be no structural problem, but the pain is very real—and mental health plays a major role in recovery.
What Helped Me
Reducing fear and anxiety (therapy, CBT if needed)
Consciously relaxing pelvic floor muscles at rest, during urination, and during intercourse
Deep diaphragmatic breathing
Wearing loose clothing and minimizing friction
Avoiding unnecessary creams, gels, and medications
Gentle vulvar hygiene using cool water; avoiding soap and hot water
Staying hydrated and supporting healthy bacteria with fermented foods
Treating confirmed infections thoughtfully, based on cultures
Fully relaxing during urination to avoid residual urine
Avoiding fragranced or irritating sanitary pads
Lying on my stomach, which helped relax pelvic muscles
Healing was slow. It required patience, psychological effort, and relearning trust in my body.
What I Want Other Women to Know
Vulvodynia is real.
Pain without visible findings is still pain.
And recovery is possible.
You have to slowly convince your nervous system that you are safe—that your body is not broken. Healing doesn’t come from force, but from understanding.
At Whuman, we believe stories like this matter. Because clarity is often the first step towards healing.